Senescent Cell Physiology Overview
Cellular senescence is a physiological process wherein there is a permanent growth inhibition of old and/or damaged cells. Scientists have dubbed these cells ‘zombie cells’ for the fact that they are damaged but don’t technically die. They exist in response to a variety of stressors, including but not limited to genotoxic, oxidative and oncogenic stress, as well as radiation, chemotherapeutics, and mitochondrial malfunction. Many changes within these cells take place including metabolic remodeling but perhaps the most clinically significant being the secretion of a myriad of proinflammatory mediators which are collectively referred to as senescence-associated secretory phenotype (SASP).
Under normal conditions, old and/or damaged cells (Initiated cell) are eliminated by apoptosis (a word derived from the Greek meaning “falling off,”) which is a form of programmed cell death. When this first mechanism of protection fails, old and/or damaged cells go senescent with permanent growth inhibition and resistance to apoptosis most likely through the overexpression of the Bcl-2 protein. Because senescent cells would resist programmed cell death, invariably this would lead to the accumulation of these cells within tissues.
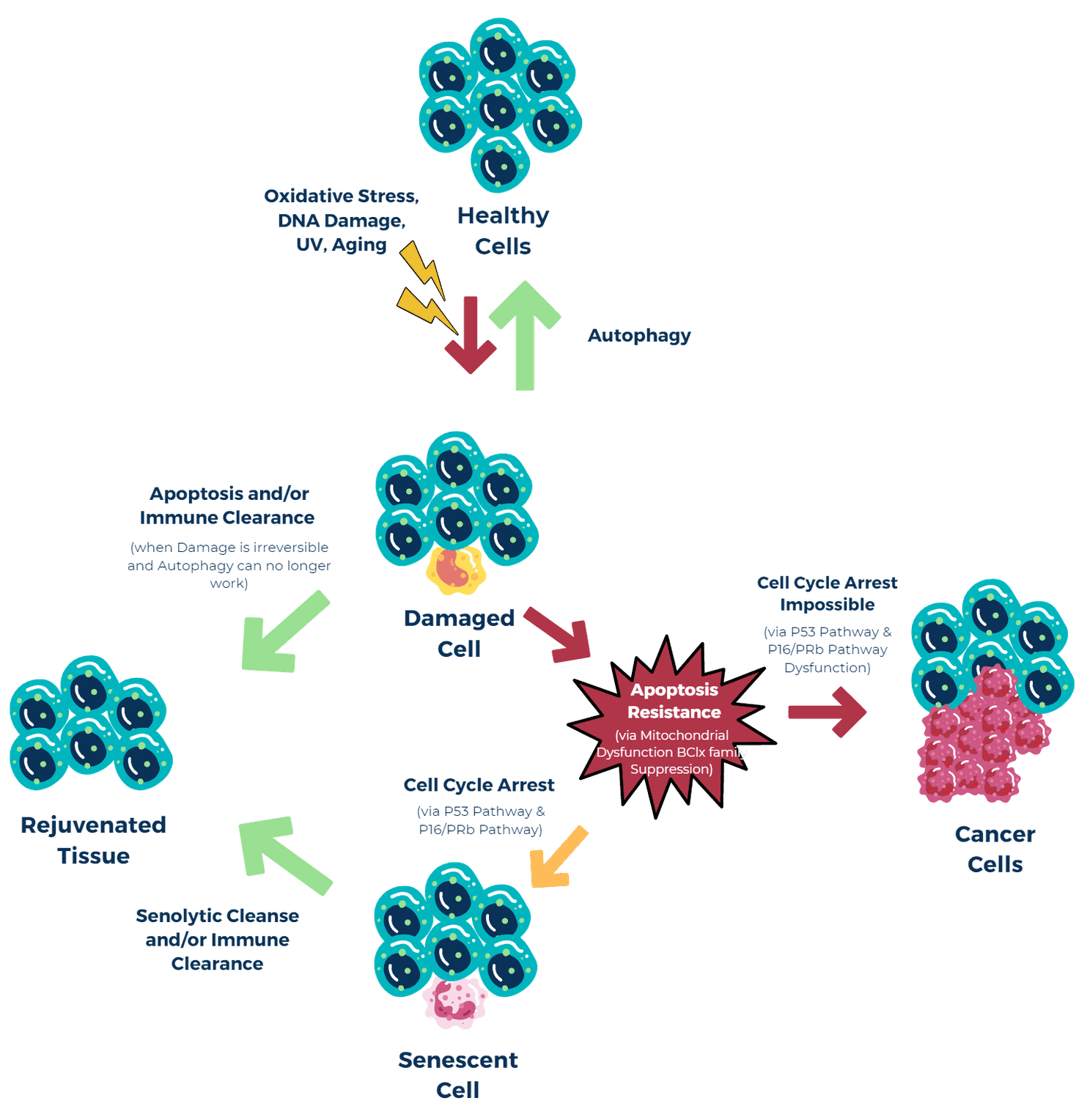
These senescent cells play a critical role in cellular homeostasis by inhibiting the proliferation of abnormal cell growth thus preventing neoplastic transformation. In fact, cancer cells must somehow bypass senescence, i.e., through inactivation of p53, p16, pRb and/or activation of telomerase, in order to continue proliferating. This system works incredibly well unless in the prevention of cancerous growth, however, where there is an excess accumulation of these zombie cells, a variety of pathological conditions can result including age related disorders and, ironically, cancer.
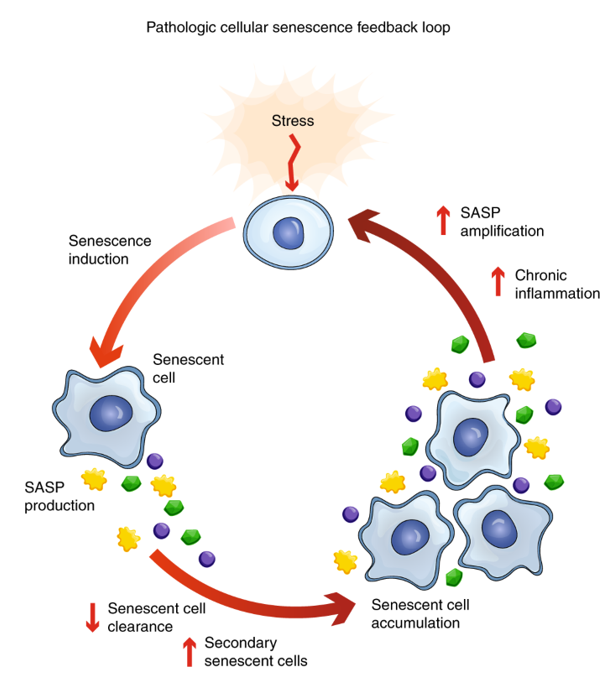
In fact, this double-edged sword is driven by SASP in that under the normal conditions, SASP induces an autocrine positive feedback loop, which inhibits aberrant cell growth and stimulates tumor suppression processes. However, the increase in secretion of the proinflammatory mediators can trigger transformation of premalignant cells to malignant, proliferation of premalignant epithelial cells and tumor vascularization. Therefore, the need to prevent accumulation is an area that needs to be addressed in practice to optimize clinical patient outcomes.

Senolytic Science Part I